Aotearoa New Zealand (NZ’s) Alert Level system worked well in 2020, but the Covid-19 landscape is changing and the system needs to change with it to keep NZ ahead of the pandemic. In this blog we summarise our just-published recommendations for strengthening the Alert Level system and describe the benefits of an upgraded system: to better protect us from outbreaks, avoid lockdowns, help us transition to a post-vaccination future, support prevention of other respiratory disease epidemics, and uphold Te Tiriti o Waitangi.
On 19-21 June 2021 NZ experienced a critical incident in which a traveller with Delta-variant Covid-19 infection visited numerous crowded indoor venues in Wellington. The visitor only transmitted the infection to their partner who was travelling with them, and NZ was spared what might have been a series of super-spreading episodes that could have stretched our contact tracing system and required an intense lockdown to contain. This incident is one of several warnings that we need an upgraded Alert Level system.
In our recent paper in the journal Lancet Regional Health: ‘Expansion of a national Covid-19 alert level system to improve population health and uphold the values of Indigenous peoples’1 we describe actions that can be taken to address several warning signals about gaps in our pandemic response. Here are five reasons we need to upgrade our Alert Level system now:
1. Science is telling us we need to revise our Alert Level system
Uncontrolled Covid-19 transmission in countries outside NZ is driving the emergence of new variants that are increasingly transmissible and may evade protection by current vaccines. In practice this means that true collective immunity will be difficult to achieve using vaccines alone. To navigate the new variant phase of the pandemic we need to have vaccination and public health and social measures working together, particularly while the majority of New Zealanders are unvaccinated.
The Alert Levels also need to be updated to reflect what is now known about the importance of airborne transmission. There have been several warnings recently in the form of transmission within hotel-based quarantine in Australia and New Zealand.2 The proposed upgrade adds control measures including wearing masks (face coverings) in settings where the risk of transmission may be high, optimising ventilation and filtration systems, and recognising that the risk of transmission via inhalation is much lower outdoors than indoors. These measures will also provide protection against a number of non-Covid infectious diseases as outlined in item 4 below.
2. Stopping outbreaks without lockdowns requires a more nuanced Alert Level system
When the Sydney traveller tested positive the Government announced that Wellington would move up to Alert Level 2. At this level schools, businesses, and other venues including hospitality and recreation remained open with minimal indoor mask use (it was voluntary). Given the high transmissibility of the Delta variant it seems unlikely that Alert Level 2 settings would have contained an outbreak of this variant if further transmission had occurred. On the other hand, there was likely to have been resistance to moving up to Alert Level 3 (lockdown) given that the case had already returned to Australia and there were no detected cases in the community in Wellington.
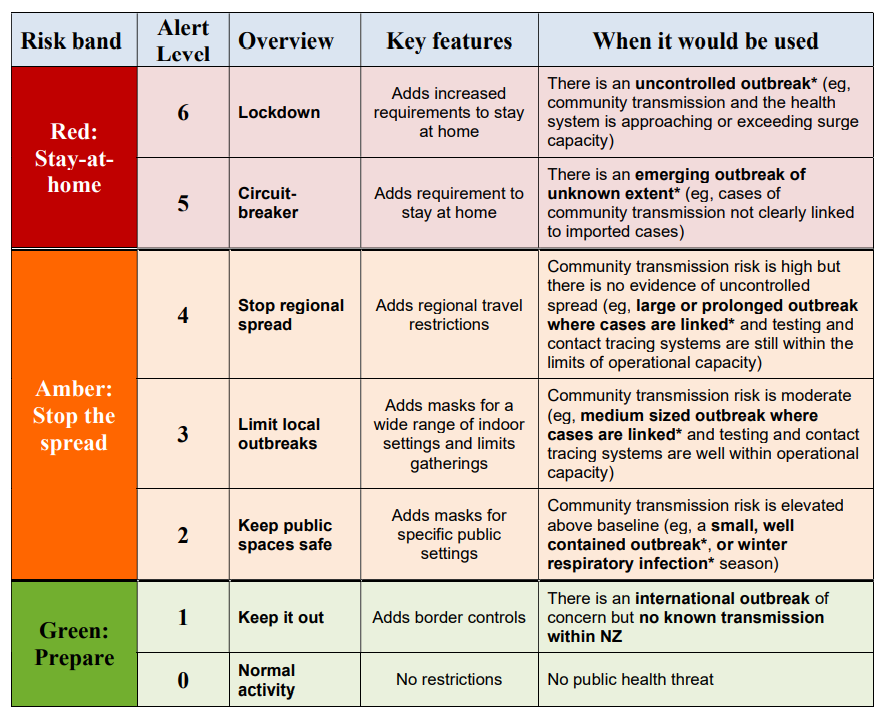
Table 1 shows what an expanded Alert Level system could look like, allowing a more tightly calibrated response to the outbreak risk posed by the Sydney traveller. In the proposed system there are six levels (plus a zero level as in the current four-level system) but the public would not need to memorise these levels. Instead, when the Sydney case was identified the public would have been informed that the risk level was now ‘amber’ and they would be required to adhere to specific requirements regarding masks, gathering sizes, and travel. In view of the high potential risk that superspreading events may have occurred (given the locations of interest), a move to the top level of the amber risk zone would probably have been justified to generate meaningful prevention of community transmission while contacts were being tested and the situation was being assessed. The rest of NZ could potentially have been moved to the bottom of the amber scale to indicate heightened concern, but with minimal impact on normal activities.
3. We need an Alert Level system to support our transition into a post-vaccination future
It is clear that vaccines are a tremendous asset to the elimination strategy but we will probably not be able to vaccinate our way out of the pandemic. Instead, a comprehensive approach is needed that makes effective use of all of our control measures in carefully calibrated ways. An upgraded Alert Level system could provide a basis for transitioning into the future with an increasingly well-vaccinated population and a simple basis for increasing controls on virus transmission if needed. This system would be an enduring legacy of the pandemic, ready to respond to a future threat such as emergence of a novel, severe pathogen or a new pandemic.
4. The Alert Level system should provide protective measures for other endemic, epidemic, and pandemic infectious diseases
The current ‘double winter season’ of RSV infection in young children is a concerning signal that heralds the likely return of a number of infectious diseases that are also spread by respiratory transmission, including meningococcal disease. Their elimination or near-elimination during the winter of 2020 indicates that much of the winter respiratory infectious disease burden is preventable. Strengthening the base levels of the Alert Level system to prevent Covid-19 outbreaks can thus potentially deliver multiple co-benefits for population health.
In the case of RSV, infants commonly acquire this infection from older siblings attending school.3 A key action for prevention of an array of non-Covid infections including RSV is the promotion of a strong culture of staying home when unwell, which is a feature of the proposed system at all levels. It is critical that public health messaging about staying home is underpinned by additional support in the form of paid sick leave provision to allow all workers, including those who are self-employed or undertaking casual work, to stay at home when they or their children are ill.
5. The Alert Level system should uphold Te Tiriti o Waitangi
Indigenous peoples experience significantly higher risk of adverse health outcomes from Covid-19 infection.4 The Government’s Covid-19 elimination strategy is therefore equity-promoting in principle; but in practice Māori have been excluded from key decisions regarding their health as highlighted by Te Rōpū Whakakaupapa Urutā/The National Māori Pandemic Group (https://www.uruta.maori.nz) and others (see the supplementary materials in our published paper).
Aotearoa New Zealand’s stringent pandemic response measures, particularly the Alert Level 4 lockdown in 2020, have generated severe hardship for some communities and have notably worsened pre-existing food insecurity and hunger.5 Many have experienced considerable distress through being unable to attend funerals/tangihanga. The Alert Level system needs to build in harm reduction measures proportionate to the stringency of control measures at every level. Examples include resources for community food sovereignty (Māra Kai/community food gardens) and development of culturally appropriate protocols for funerals and tangihanga that protect both tikanga Māori and the pandemic safety of whānau at these gatherings.
Conclusions
We cannot continue to ignore numerous warning signs indicating that NZ is currently at high risk of a Covid-19 outbreak and its consequences, as well as being at risk of other infectious disease outbreaks. An immediate upgrade of the Alert Level system by the Government would offer multiple opportunities to incorporate new scientific knowledge, strengthen our response, and protect population health as the Covid-19 pandemic continues to evolve and we face new challenges such as an RSV epidemic.
Table 1. Summary of the proposed revised Alert Levels for future management of the Covid-19 pandemic and other infectious disease outbreaks. This system is optimised for infections with similar transmission characteristics to SARS-CoV-2 and may need to be adapted to respond to other infections, including those transmitted by other routes (eg, direct contact as in Ebola).
* Of Covid-19 or another pathogen that is highly transmissible and has moderate to high illness severity.