New Zealand Health Survey (NZHS) data released in early December suggest substantial reductions in smoking prevalence occurred between 2019/20 and 2020/21 among all ethnic groups. This blog describes the key findings, explores the data in more detail, and discusses how these changes may have arisen and their implications, particularly given the Government has now released an innovative Action Plan outlining how it will achieve the Smokefree Aotearoa goal.
Introduction
In previous years we prepared blogs summarising key points from the 2018/19 and 2019/20 NZ Health Surveys (NZHS), a rolling survey conducted every year since 2011/12. These analyses revealed a steady but unspectacular decrease in smoking prevalence since 2011, continuing a gradual decline going back several decades. Data from 2011/12 to 2019/20 also showed persisting large disparities in smoking by ethnicity and socio-economic status (SES). We concluded, and modelling studies provided supporting evidence,1 that the government was not on track to achieve the Smokefree Aotearoa 2025 goal for all population groups.
The 2020/21 NZHS collected data on smoking and e-cigarette (EC) use from a nationally representative sample of 9709 adults aged 15 years and over between September 2020 and August 2021. Full details of the methods are available on the Ministry of Health website. The findings reveal a different picture from previous surveys, with the Ministry of Health reporting that the decline in smoking evident in 2020/21 was much larger than in previous years.
This blog explores the 2020/21 survey data to assess patterns of change in smoking prevalence, investigate factors potentially driving the reported decrease in prevalence, and examine possible implications of these changes. The data has been sourced from the NZHS data explorer. All figures presented in the graphs and reported in the text are uneless otherwise stated crude (unadjusted) prevalences with no adjustment for age or other demographic variables.
Key Findings
1. Overall smoking prevalence and e-cigarettes use trends
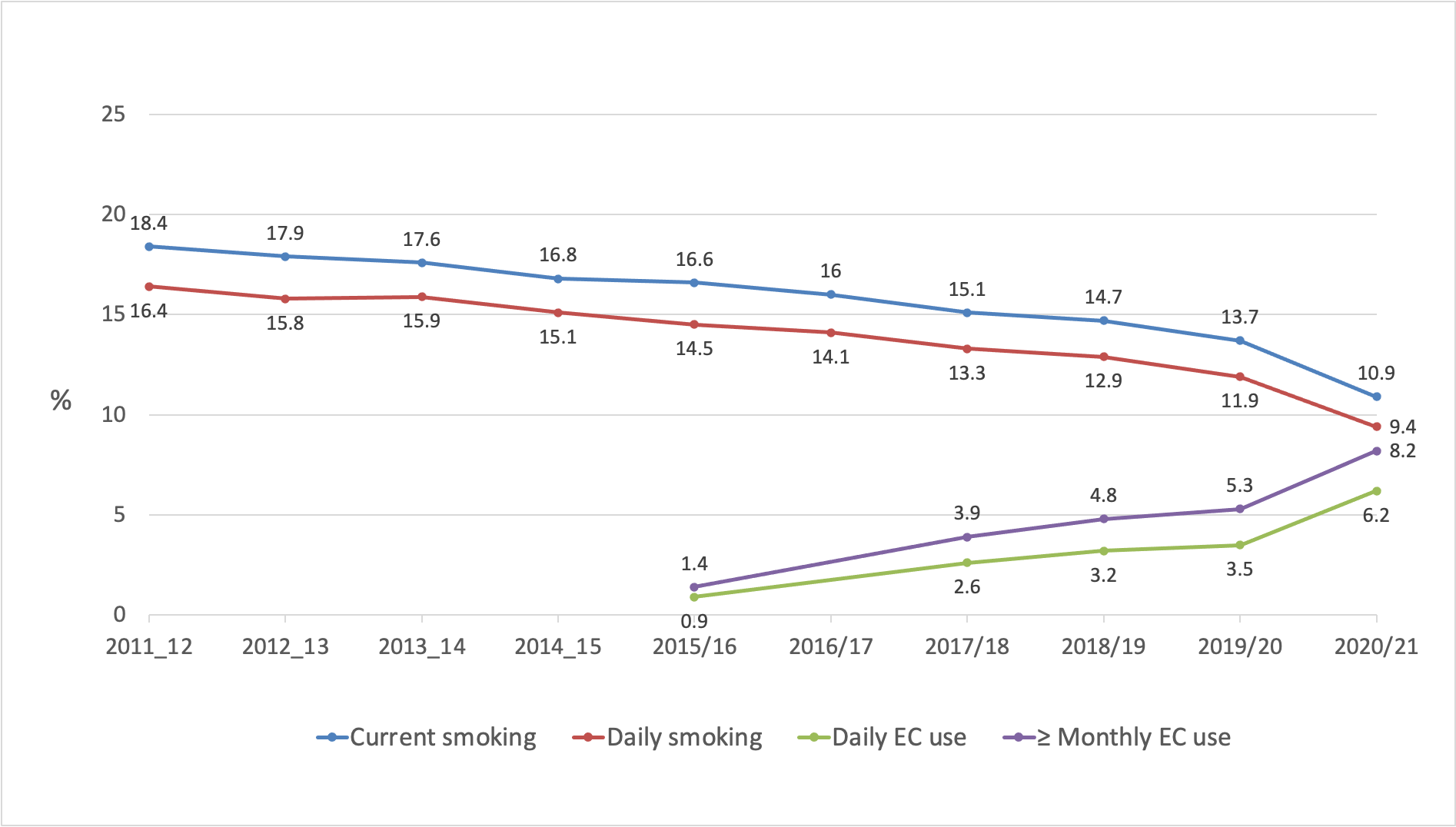
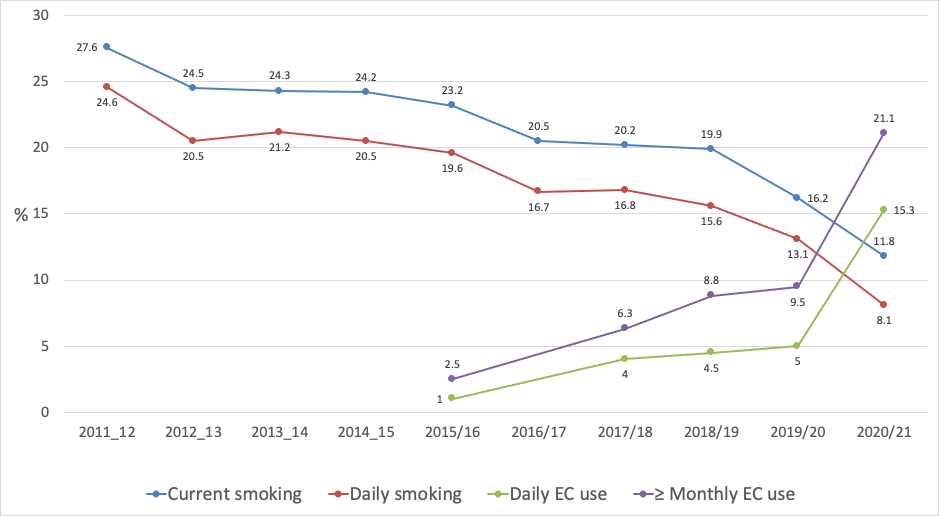
Figure 1 shows the trends in current (at least monthly) and daily smoking prevalence and prevalence of current (at least monthly) and daily use of ECs each year between 2011/12 and 2020/21.
Daily smoking prevalence in 2020/21 was 9.4% (95%CI: 8.7-10.1%) representing an estimated 387,000 people. Current (at least monthly) smoking prevalence was 10.9% (95%CI: 10.1-11.7%), representing 451,000 people. There was a steady, though unspectacular, decline in current and daily smoking prevalence of about 0.6% per year in absolute terms from 2011/12 to 2019/20. However, from 2019/20 to 2020/21, daily smoking prevalence fell by 2.5% and current smoking prevalence by 2.8%.
Figure 1 Trends in current (≥monthly) and daily smoking and e-cigarette use (NZHS 2011/12 to 2020/21)
Use of ECs was first assessed in 2015/16; since then, the prevalence of current and daily EC use has steadily increased. The increase in EC use was much greater in 2020/21: current EC use grew from 5.3% in 2019/20 to 8.2% in 2020/21 and daily EC use from 3.5% to 6.2% over the same period. The increase in daily and current EC use between 2019/20 and 2020/21 occurred concurrently with the large reduction observed in smoking prevalence (Figure 1), whereas the more gradual increase in EC use between 2015/16 and 2019/20 was not associated with a substantial change in the rate of decline in smoking prevalence.
2. Smoking and e-cigarette use by age and gender
Daily (9.5% men vs 9.2% women) and current (11.6% men vs 10.2% women) smoking prevalence in 2020/21 were similar for men and women. Since 2018/19, absolute decreases in current (4.5% men vs 2.2% women) and daily (4.9% men vs 2.3% women) smoking prevalence have been greater among men. E-cigarette use was slightly higher among men in 2020/21 – current EC use 9.5% for men vs 7.0% for women and daily EC use 7.5% for men vs 5.0% for women.
Smoking is strongly patterned by age. In 2020/21, current smoking prevalence was low (1.4%) among 15-17 year olds, and much higher (11.8%) in the 18-24 year old age group, with similar levels (12.5-14.6%) in all age groups to 55-64 years. Prevalence was lower among older adults – 6.2% among 65-74 year olds and 2.6% among people aged 75 years or over.
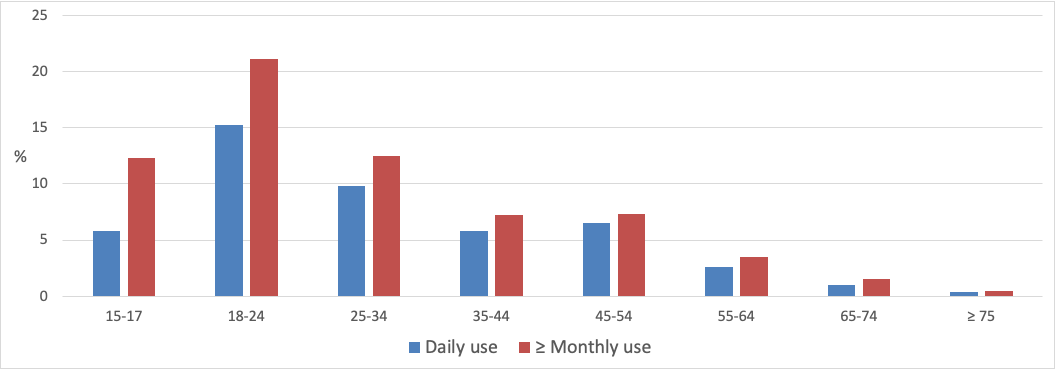
EC use also varies greatly with age (Figure 2), and is most prevalent among 18-24 year olds (15.3% daily, 21.1% current) but relatively rare among people aged 55 years or older.
Figure 2 Daily and current (≥ monthly) e-cigarette use by age group (NZHS 2020/21)
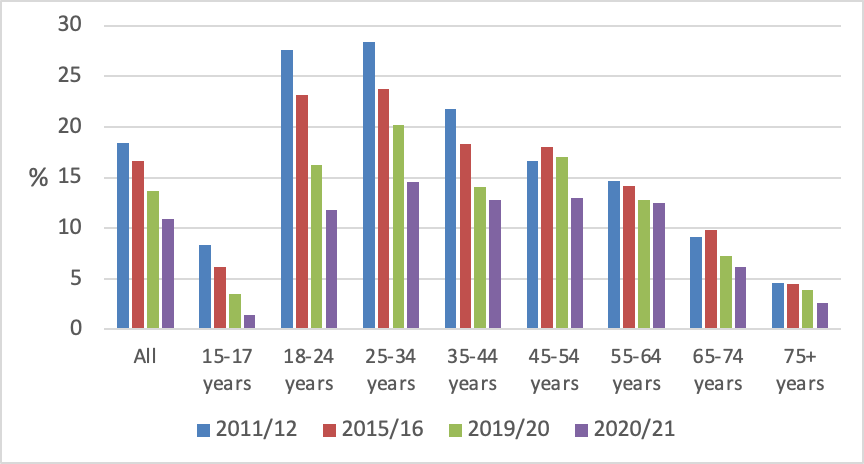
Figure 3 shows changes in current smoking prevalence over time by age group since 2011/12. Reductions in smoking prevalence were greatest in absolute terms for the 18-24 and 25-34 year age groups, and also declined to very low levels (1.4%) among 15-17 year olds. Smoking prevalence reductions were smaller in older age groups, particularly among people aged 55 years and over.
Figure 3 Current smoking prevalence by age group (NZHS 2011/12, 2015/16, 2019/20 and 2020/21)
Figures 4 and 5 present trends in current and daily smoking prevalence among 15-17 year olds and 18-24 year olds.
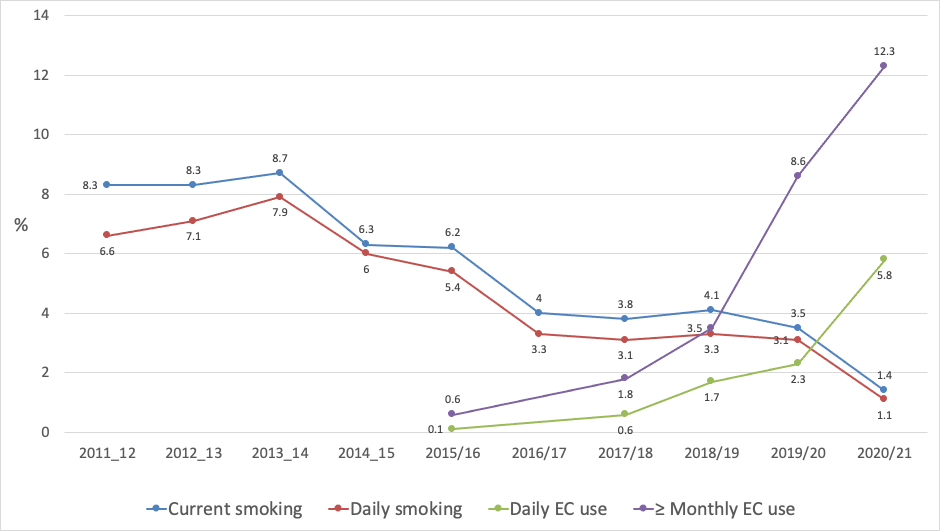
Figure 4 Trends in current and daily smoking and e-cigarette use among 15-17 year olds (NZHS 2011/12 to 2020/21)
Current and daily smoking prevalence among 15-17 year olds approximately halved between 2011/12 and 2016/17, but then showed little change until 2020/21, when it declined by almost 2% in absolute terms to 1.4% current and 1.1% daily smoking prevalence (Figure 4). Conversely, prevalence of EC use increased each year from 2015/16 reaching 3.5% for current EC use in 2018/19 and thereafter more than tripled to 12.3% by 2020/21. Daily use increased gradually to 2.3% by 2019/20, but then more than doubled to 5.8% in 2020/21.
Figure 5 Trends in current and daily smoking and e-cigarette use among 18-24 year olds (NZHS 2011/12 to 2020/21)
Similar patterns were apparent for 18-24 year olds (Figure 5). Current and daily smoking prevalence among 18-24 year olds decreased gradually between 2012/13 and 2018/19, since when it has declined rapidly, with the biggest falls of over 4% in absolute terms occurring between 2019/20 and 2020/21. E-cigarette use prevalence increased steadily from 2015/16 reaching 9.5% for current EC use in 2019/20 and thereafter more than doubled to 21.1% by 2020/21. Daily use increased gradually to 5.0% by 2019/20, but then trebled to 15.3% in 2020/21.
Figures for smoking and EC use among young adults by ethnicity are not available in the NZHS data explorer.
The data presented in Figures 4 and 5 suggest some substitution of EC use for smoking has occurred. However, the increase in prevalence of current EC use from 2018/19 to 2020/21 for 15-17 year olds and from 2019/20 to 2020/21 for 18-24 year olds was much larger than the reduction in the prevalence of current smoking. This finding suggests many current EC users in these age groups were never smokers who would not have become current smokers and therefore that the prevalence of current use of any nicotine product (cigarettes or ECs) among these age groups increased during these time periods.
However, it is difficult to quantify this increase using these data as simply summing current smoking and EC use prevalences will over-estimate prevalence of any nicotine product use. This is because people who smoke and use ECs (dual users) will be included in the calculation of both current smoking and current EC use prevalence. The NZHS Explorer data does not identify the proportion of people who are dual users, so the extent to which summing smoking and EC use prevalences over-estimates any nicotine product use cannot be calculated.
3. Smoking and e-cigarette use by ethnicity
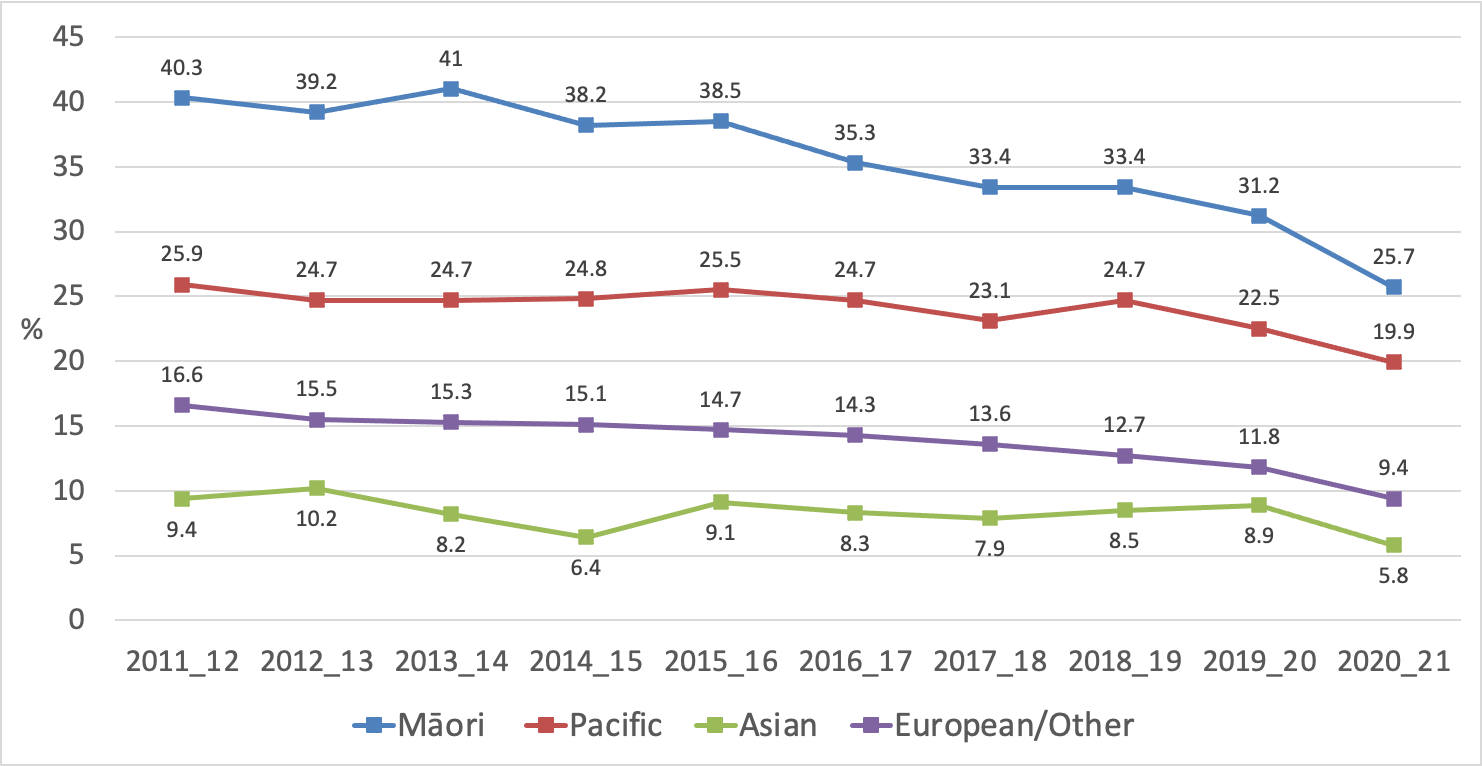
Figures 6 and 7 show the trends in current and daily smoking prevalence by ethnicity. Substantial disparities persist, although absolute differences in prevalence narrowed in 2020/21, particularly for Māori compared to European/other.
There was a substantial decline in Māori current smoking prevalence from 31.2% in 2019/20 to 25.7% in 2020/21. The decrease was greater among women e.g., current smoking prevalence fell from 35.0% to 25.8% while men showed a smaller decline from 27.3% to 25.6%. The absolute difference in current smoking prevalence between Māori and European/others narrowed by 3.1% between 2019/20 and 2020/21.
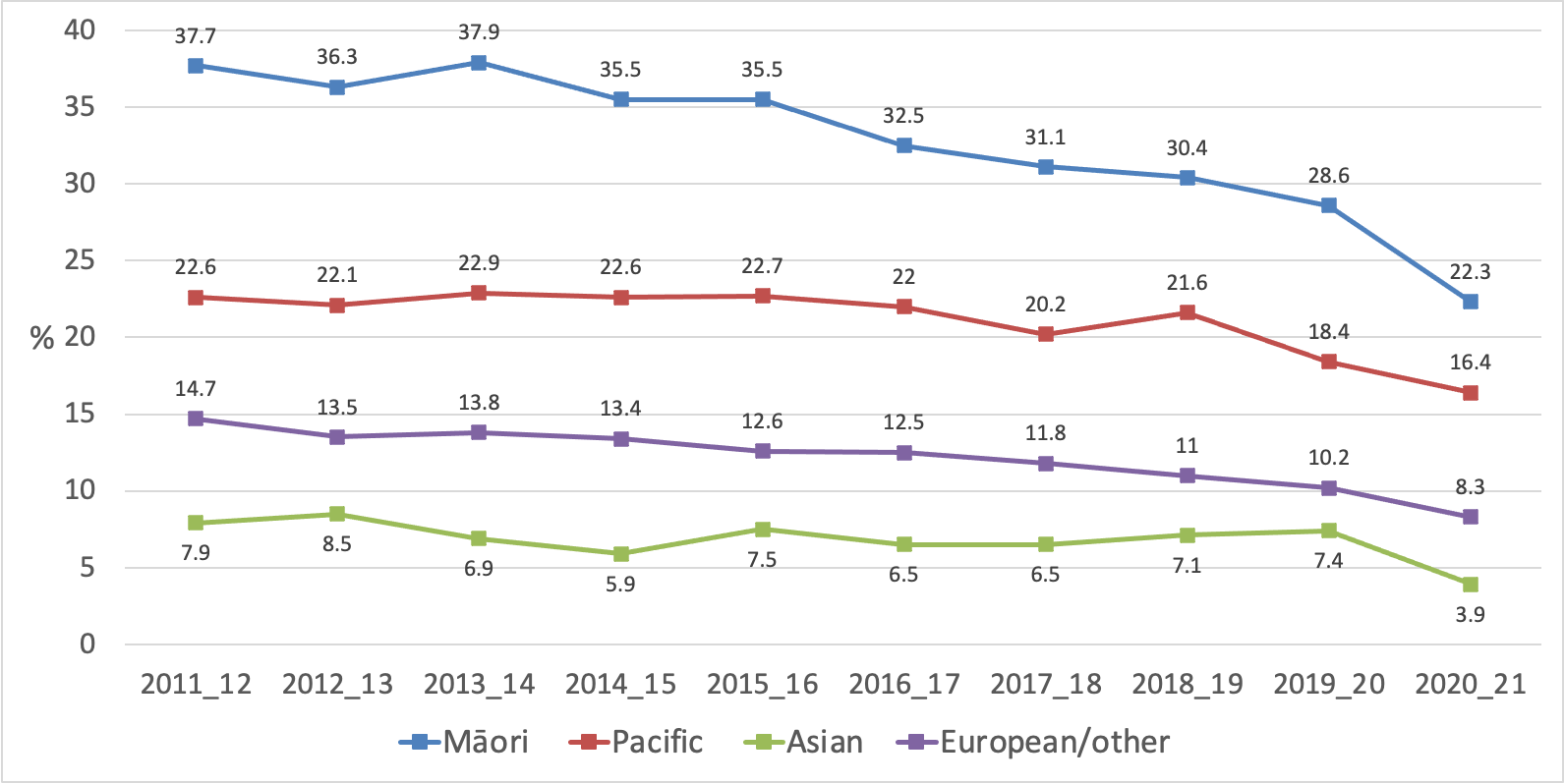
Similarly, Māori daily smoking prevalence declined from 28.6% in 2019/20 to 22.3% in 2020/21, with larger decreases among women. The absolute difference in daily smoking among Māori compared to European/others narrowed by 4.4%.
The decreases in Māori current and daily smoking prevalence in 2020/21 were more than twice as large as for any other years since 2011/12. However, relative differences in prevalence did not change appreciably. For example, Māori were three times more likely than non-Māori to be daily smokers – prevalence ratio: 3.06, 95%CI: 2.69-3.48, adjusted for age and gender (this ratio was unchanged from 2019/20).
Pacific peoples current smoking prevalence decreased from 22.5% in 2019/20 to 19.9% in 2020/21 and daily smoking prevalence declined from 18.4% in 2019/20 to 16.4% in 2020/21. In contrast to Māori, the fall in prevalence among Pacific peoples occurred predominantly in men, where current smoking prevalence fell from 26.8% to 20.3%. Prevalence was essentially unchanged for women: 19.0% in 2019/20 and 19.5% in 2020/21.
The relative and absolute differences in current and daily smoking compared to European/others were largely unchanged in 2020/21 compared to 2019/20. Pacific peoples were more than 1.8 times (prevalence ratio: 1.81, 95%CI: 1.42-2.31, adjusted for age and gender) more likely than non-Pacific people to be daily smokers.
Figure 6 Trends in current smoking prevalence by ethnicity (NZHS 2011/12 to 2020/21)
Figure 7 Trends in daily smoking prevalence by ethnicity (NZHS 2011/12 to 2020/21)
Finally, for the first time since 2011/12, there was a substantial decrease in smoking prevalence among Asian peoples in 2020/21. This change was driven largely by falls in prevalence among men (e.g. current smoking changed from 14% to 9%).
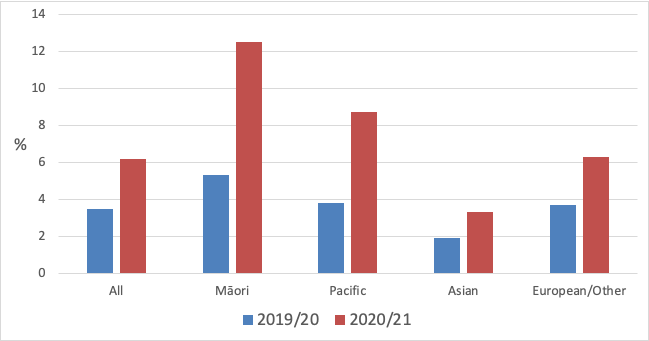
There were also differences in EC use by ethnicity (Figure 8), with substantial increases among Māori and Pacific peoples between 2019/20 and 2020/21. The increase in EC use among Māori was greater among men (daily EC use increased from 5.4% to 15.2% for men and from 5.3% to 10.0% for women), but was similar for men and women among Pacific peoples (daily EC use increased from 5.7% to 11.7% for men and from 2.3% to 6.3% for women).
Figure 8 Daily e-cigarette use by ethnicity (NZHS 2019/20 and 2020/21)
4. Smoking prevalence and e-cigarette use by socio-economic status
There are very large disparities in smoking by SES (as measured by NZDep, an indicator of neighbourhood deprivation) (Figure 9).
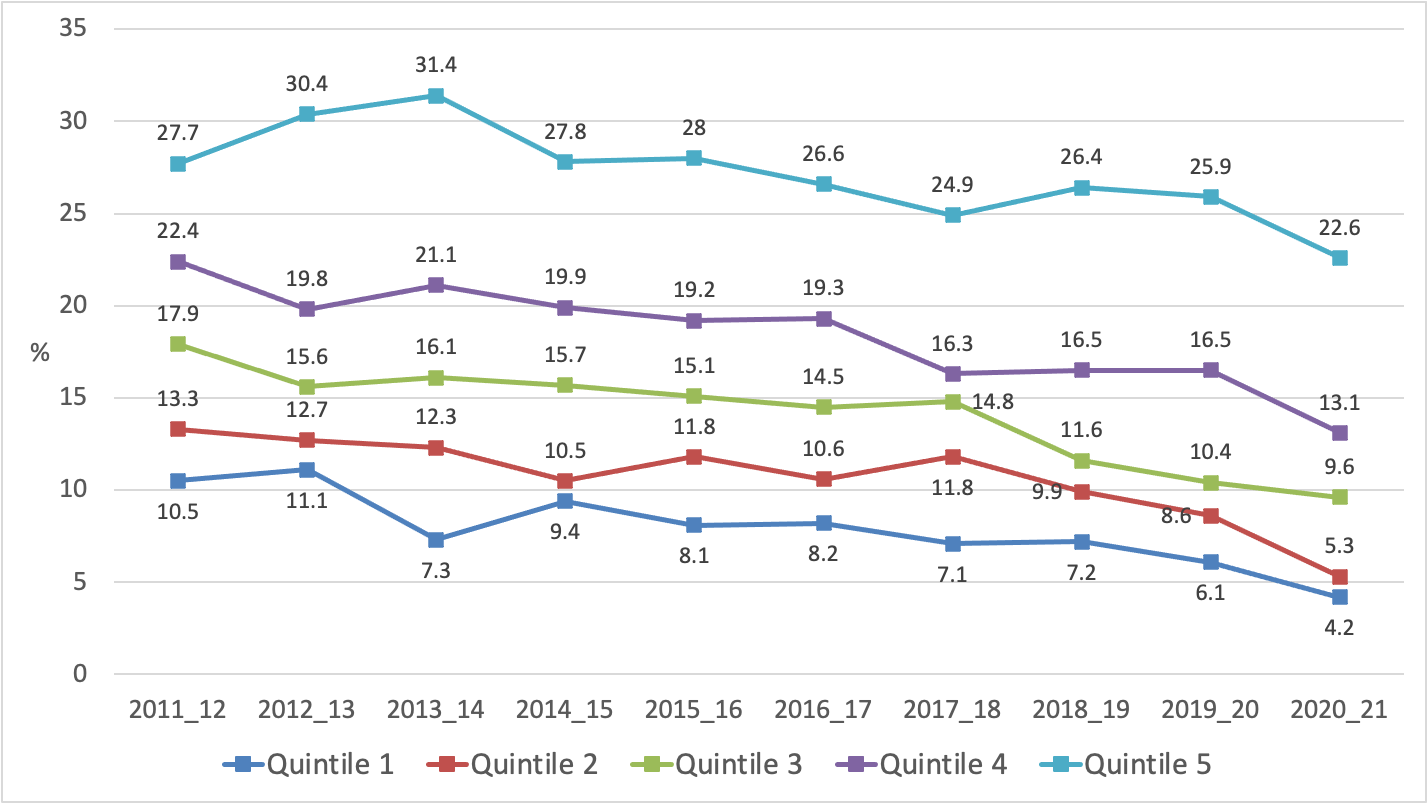
Current smoking prevalence in 2020/21 was over six times (prevalence ratio: 6.06, 95%CI: 4.22 to 8.70, adjusted for age, gender and ethnicity) higher among the most deprived quintile of the population (quintile 5: 22.6%, 180,000 people) than the least deprived quintile (quintile 1: 4.2%, 35,000 people). Daily smoking was over seven times higher (prevalence ratio: 7.20, 95%CI: 4.92 to 10.53, adjusted for age, gender and ethnicity) in the most deprived quintile (20.0%, 159,000 people) than in the least deprived quintile (3.4%, 28,000 people).
However, Figure 9 shows that, in 2020/21, substantial reductions in current smoking (3.3% absolute reduction) occurred among the most deprived quintile for the first time since the 2014/15 survey. There was also a large (3.6% absolute reduction) decline in daily smoking in this quintile in 2020/21.
E-cigarette use also varied with SES, with the highest use among people living in the most deprived areas. Daily use was 3.2% (an increase from 2.2% in 2019/20) among NZDep quintile 1 increasing to 8.6% in the most deprived group (quintile 5; up from 5.2% in 2019/20). Similarly, current EC use varied from 4.9% in quintile 1 to 11.9% in quintile 5.
Figure 9 Trends in current smoking prevalence by socio-economic status (NZDep) (NZHS 2011/12 to 2020/21 with quintile 5 being the most deprived)
5. Quit rates
The NZHS estimates smoking quit rates using the number of people who reported they had quit smoking in the last year and had been quit for at least a month. These figures will over-estimate long term quit rates as some recent quitters will subsequently relapse to smoking and self-reported figures may over-estimate true quit rates. The quit rates are for quitting smoking, but not necessarily quitting all nicotine product use: some recent quitters will have switched to ECs. The proportion of quitters who have switched to ECs is not available in the data explorer.
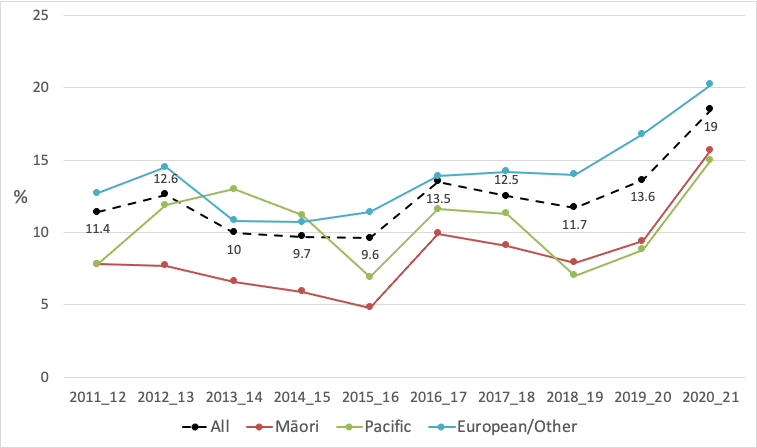
Figure 10 shows that overall quit rates varied between 9.6% (2015/16) and 13.6% (2019/20) during the period from 2011/12 and 2019/20, but increased markedly to 19.0% in 2020/21. There were also large increases in quit rates for all ethnic groups in 2020/21; with particularly large increases among Māori (9.4% in 2019/20 vs 16.0% in 2020/21) and Pacific peoples (8.8% vs 15.0%). However, quit rates were higher among European/other people than among Māori and Pacific peoples in 2020/21, as they have been every year since 2011/12 for Māori, and since 2015/16 for Pacific.
Figure 10 Trends in quit rates by ethnicity # (NZHS 2011/12 to 2020/21)
# Quit rates among Asian peoples are not reported in this graph as these fluctuated widely, possibly reflecting chance variations due to the smaller numbers of participants identifying with Asian ethnicities.
In 2020/21, quit rates varied substantially by SES (Figure 11) and age group (Figure 12).
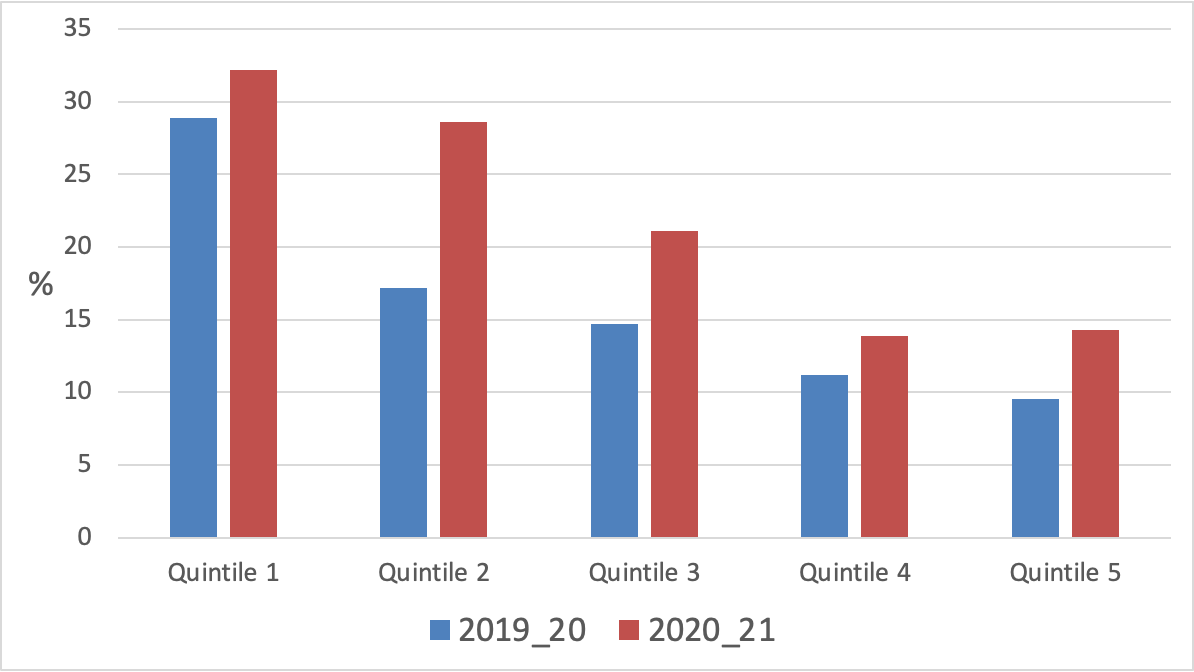
Figure 11 shows that the socio-economic gradient in quit rates increased in 2020/21 – quit rates were twice as high among people who smoke from the most affluent areas (NZDep quintiles 1 and 2) compared to those living in the most deprived areas (NZ Dep quintiles 4 and 5).
Figure 11 Quit rates by socio-economic status (NZDep) (NZHS 2019/20 and 2020/21 with quintile 5 being the most deprived)
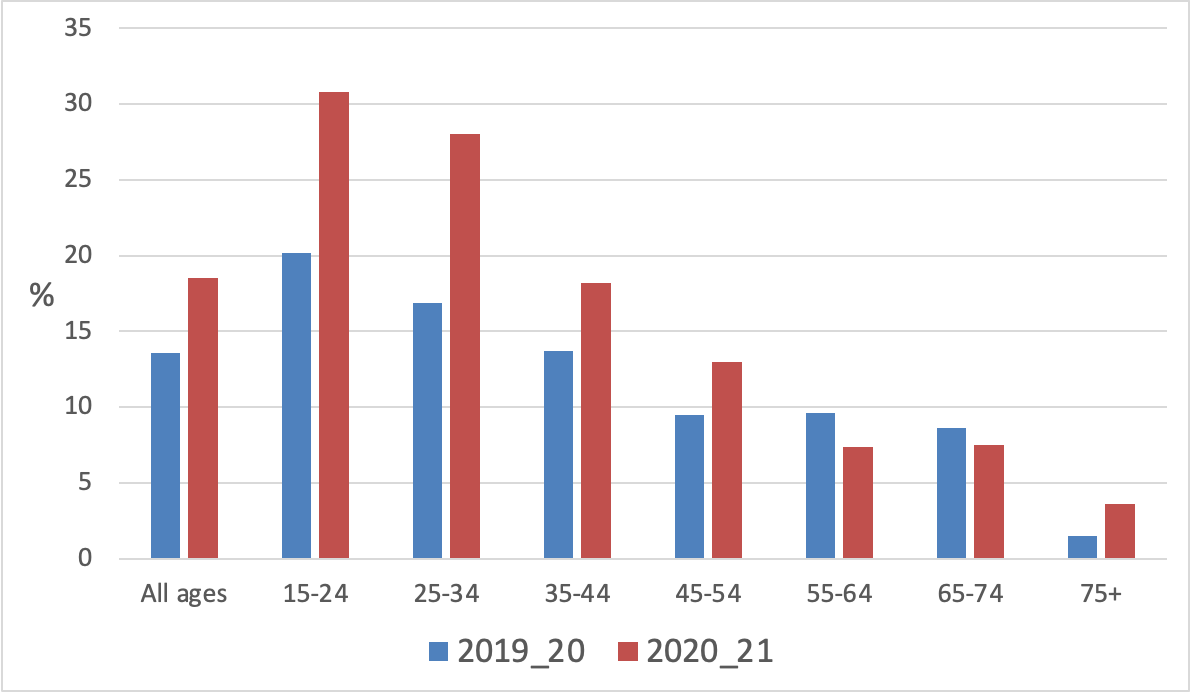
Figure 12 shows that quit rates decrease greatly with age, and this age-related quitting gradient increased in 2020/1. Leaving aside the 15-24 year old group (high ‘quit rates’ may reflect frequent cycling between smoking and being quit in this age group), there was a seven fold variation in quit rates from 28% among 25-34 years to less than 4% among over 75 year olds. Quit rates increased most in 2020/21 among younger age groups, but changed much less among people who smoke aged 55 or older.
Figure 12 Quit rates by age group (NZHS 2019/20 and 2020/21)
Commentary
The key findings from the 2020/21 NZHS include the following:
- There was a substantial reduction in daily and current smoking prevalence in 2020/21, including among Māori and Pacific peoples, although large disparities by ethnicity and SES remain
- The reduction in smoking prevalence was mirrored by a big increase in quit rates in 2020/21
- The greatest reduction in smoking prevalence throughout the 2011/12 to 2020/21 period and between 2019/20 and 2020/21 occurred among people aged <35 years, with much smaller reductions among people aged ≥55 years
- There was a large increase in prevalence of daily and current EC use, with the increase greatest among young people aged <25 years
The reductions in smoking prevalence observed in 2020/21 are very encouraging, and if maintained at the same rate would result in minimal smoking prevalence by 2025, including among Māori and Pacific peoples. However, caution is required when interpreting survey data and extrapolating trends from a single survey year.
The first question to ask when large changes are observed in health measures between surveys is whether the findings could be due to chance or affected by biases.
Chance findings due to random variations in sampling are always a possibility in survey research. The risk of a chance finding are slightly greater as there were fewer participants in the 2020/21 survey (around 9700 vs approximately 14,000 from 2011/12 to 2019/20) than in previous years due to the impact of the COVID-19 pandemic. However, the sample size is still large and the precision of the estimates remained reasonably high, though caution is need for smaller subgroups such as 15-17 year age band, Pacific and Asian ethnicities. Evidence from future surveys will be needed to assess whether the results in 2020/21 indicate a chance effect or mark a real and sustained change.
The NZHS is carried out each year using largely consistent methods. The most plausible threat from bias is that the COVID-19 pandemic resulted in a systematic change to the methods e.g., to the sampling strategy, participation rates or to the data collection methods. Again, this explanation seems unlikely. There were no major changes to the methods other than a small number (n=31) of interviews were conducted by video rather than all being face-to-face (as in previous surveys). The Ministry survey team (personal communication) noted that the sample’s demographic characteristics did not differ greatly from previous years. If the 2020/21 NZHS participants were systematically different from previous surveys, then substantial changes might be expected in multiple measures included in the survey, particularly in other health-related behaviours. However, this was not the case. For example, the prevalence of hazardous and problem drinking was largely unchanged in 2020/21 compared to 2019/20.
Furthermore, the 2020/21 NZHS findings are consistent with other surveys conducted over a similar time period. The Te Hiringa Hauora/Health Promotion Agency Health and Lifestyle Survey (HLS) also found a substantial decline in smoking prevalence and increase in EC use in the most recent survey period. For example, the HLS reported that daily smoking decreased from 12.8% in 2018 to 8.5% in 2020, while current EC use increased from 4.3% to 8.4% over the same time period.
Assuming the findings are not due to chance or greatly affected by bias, what could explain the observed decline in smoking prevalence? Answering this question will require more detailed investigation using other data sources as well as more sophisticated analyses of the NZHS data; however, we outline some preliminary observations below.
The two most likely explanations appear to be: (i) the impact of growing use of ECs in increasing quitting smoking among people who smoke or reducing uptake by substituting for smoking among young people; and (ii) an effect of the COVID-19 pandemic (e.g. increasing quitting through various possible mechanisms). Another possible explanation is that the change was due to the impact of changing social norms about smoking and the impact of current or previous tobacco control interventions.
The finding that smoking prevalence fell markedly in 2020/21 while EC use increased substantially provides the first clear population-level data to support the hypothesis that EC use is contributing to reductions in smoking prevalence in New Zealand. Further supporting evidence comes from the observation that the largest fall in smoking prevalence occurred in the younger age groups where EC use is most common and showed the largest increase in prevalence.
However, other findings provide less support for this hypothesis. For example, smoking prevalence decreased much more among Māori women than Māori men, but EC use increased more among Māori men. It is also unclear why the increase in prevalence of EC use from 2015/16 to 2019/20 was not accompanied by any great acceleration in the decline in smoking prevalence (see Figures 1 and 4), in contrast to the patterns observed between 2019/20 and 2020/21. A possible explanation for the latter finding is that newer EC technologies, such as easy to use ‘pod’ vapes and ECs using new nicotine salt technology have become more appealing and effective substitutes for smoking by offering higher and thus more ‘satisfying’ nicotine concentrations without the harshness of freebase e-liquids. However, as the NZHS does not collect data on nicotine content or type of vaping device used, this is not a hypothesis that can be explored through the NZHS data.
The NZHS Explorer site does not allow cross-tabulations, so we cannot investigate the impact of ECs further. Important questions remain unaddressed. For example, a very high rate of EC use among recent quitters (as reported in the ITC NZ study)2 would strengthen conclusions that EC use is helping many people who smoke to quit. Whilst high EC use among never smokers would support concerns that ECs have created a new generation of young people dependent on nicotine who may be at greater risk of subsequent smoking uptake.
A second possible explanation is that the COVID-19 pandemic and measures such as lockdowns, increased quitting and/or reduced smoking uptake. A qualitative study from the UK 3 and a THH/HPA survey in New Zealand 4 have identified plausible explanations for how the pandemic and lockdowns could increase smoking. For example, increased smoking could have occurred to address boredom and stress related to the pandemic and lockdown measures. By contrast, reduced frequency of smoking, increased quitting and reduced smoking initiation could come about through less frequent visits to tobacco retail outlets, less social exposure to smoking, increased concerns about cost and health impacts, greater opportunities and motivation to quit, and fewer opportunities to initiate smoking in young adults.
The limited literature available suggests that the pandemic is unlikely to have been a major reason for the dramatic decline in smoking prevalence seen in the 2020/21 NZHS. Studies, including two from New Zealand, 4 5 have found mixed responses to the pandemic and lockdowns among people who smoke or used to smoke. 6-13 Some reported reduced smoking and higher quitting salience among some people who smoke; however, the most common finding has been that people who smoke increased their tobacco consumption. Among studies examining how the pandemic affected smoking prevalence, two US studies 7 10 found no evidence of a major effect, and a UK study 13 found a modest increase in prevalence and quit attempts/success among people aged <35 years, but not among older people. The UK study authors noted that smoking prevalence data could have been affected by a large exodus of young people from the UK.
Finally, it is possible that other tobacco control measures have contributed to the reduction in smoking prevalence reported in 2020/21. However, this seems unlikely to fully explain the much larger fall in prevalence in 2020/21, as national level smokefree measures implemented during or close to the 2020-2021 period were no more extensive than in previous years. These measures included the last annual above inflation tobacco excise tax increases on January 1 2020, mass media campaigns such as the ‘Quit strong’ and ‘Vape to quit’ campaigns, and the introduction of enhanced pictorial warnings and standardised packs in 2018. Legislation to ban smoking in cars with children present was passed in May 2020, and a social marketing campaign about the law change (‘Drive smokefree for Tamariki’) began in April 2021, though implementation of the law occurred after the completion of the survey in November 2021. However, the finding of very substantial falls in smoking prevalence among Māori women suggest there was some effect of these measures, as wahine Māori were the primary target audience of the ‘Quit strong’ campaign. It is also possible that some of the fall in smoking prevalence was due to social norms which increasingly discourage smoking, and encourage and support quitting. In addition, reduced uptake during previous years is likely to explain some of the observed decline in prevalence in younger age groups.
There are at least four persisting areas of concern or uncertainty. First, substantial disparities in smoking persist by ethnicity and SES. Achieving the Smokefree Aotearoa 2025 goal equitably requires sustained large reductions in prevalence in subsequent years, particularly among Māori, Pacific peoples, and people living in the most deprived areas.
Second, the 2020/21 survey presents findings from only one year. Even assuming the estimates are valid, they may not represent a sustained trend. For example, if the reductions reflect a COVID-19 pandemic effect, that stimulus may not be present in future surveys. Also, if the main driver of the reductions was increased EC use, there is no guarantee ECs will have an impact at the same level in the future.
Third, the decline in smoking prevalence, increase in rates of quitting smoking, and increase in EC use were concentrated in younger age groups. This finding raises at least two questions: (i) how to increase quit rates among older age groups? and (ii) how to ensure that any positive effects of ECs on quitting/switching occur equally in older age groups?
Fourth, the rapid increase in EC use, with a possible increase in overall use of nicotine products (EC use + smoking prevalence combined), among young people aged < 25 years is a concern, particularly as the long term health effects and patterns of use of ECs are not yet well known (but ECs might be up to a third as harmful). The continuing decline in smoking among the 15-17 and 18-24 year old age groups does not support the ‘gateway hypothesis’ (i.e., that adolescent EC use leads to increased smoking initiation) at the population level, at least in the NZ setting. On the contrary, the findings lend some support to the ‘displacement hypothesis’ i.e., that EC use among adolescents may reduce smoking uptake. However, these data need monitoring carefully so that if a gateway effect from EC use to smoking emerges it is identified early and can be addressed with appropriate health promotion and regulatory measures.
These areas of concern raise important questions. How should we develop and implement EC policies that encourage switching among established smokers yet discourage use among non-smoking young people? What further actions will encourage and support quitting among Māori and Pacific peoples, low SES and older smokers? For example, targeted health promotion initiatives could aim to increase older (>55 years) smokers’ use of ECs as a smoking substitute and conduit to stopping all nicotine use.
At the same time, despite recent falls, high smoking prevalence among 18-24 year olds remains a concern, as does the rapid increase in EC use among young people. These findings suggest we urgently need additional measures to prevent both smoking and EC use in these age groups. Despite the new vaping legislation introduced in 2020, EC marketing continues to target young people aggressively and retail loopholes have done little to reduce young people’s access to vaping products. 14
Nonetheless, the Government’s comprehensive Smokefree action plan announced recently seems very likely to accelerate progress towards the Smokefree 2025 goal by discouraging smoking uptake, and prompting and supporting people who smoke to quit smoking or switch to ECs. If increased EC use is contributing to reductions in smoking prevalence, as the NZHS findings suggest, strong measures that reduce the appeal, availability and addictiveness of smoked tobacco products will cue more people to move to ECs and other vaping products, if they cannot quit completely.
* Author details: All authors are with ASPIRE2025 and the Department of Public Health, University of Otago, Wellington