Our just published modelling study suggests that easier access to nicotine via vaping as a replacement for tobacco smoking, will improve the health of the NZ population. The estimated health gain is about the same as 10% per annum tobacco tax increases per year for 15 years, or a national colorectal cancer screening programme. Considering all sources of uncertainty, our study supports cautious liberalisation of nicotine-containing e-cigarettes – as NZ is doing. In this blog we discuss this new study and issues that policy-makers should consider to maximise the potential health gain – and minimise risks.
Our joint NZ/Australian team used a computer simulation model to estimate the likely net health impact of liberalising access to e-cigarettes in NZ (relative to a situation where e-cigarettes containing nicotine were not legally available). The just published study (in a top epidemiological methods journal: Epidemiology [1]) took into account the various benefits of vaping (eg, the lower risk of vaping compared with smoking tobacco and increased population-level smoking cessation rates), as well as the risks (eg, some uptake of vaping by youth who would have otherwise remained smokefree and vapefree, and former smokers vaping long-term instead of staying nicotine-free).
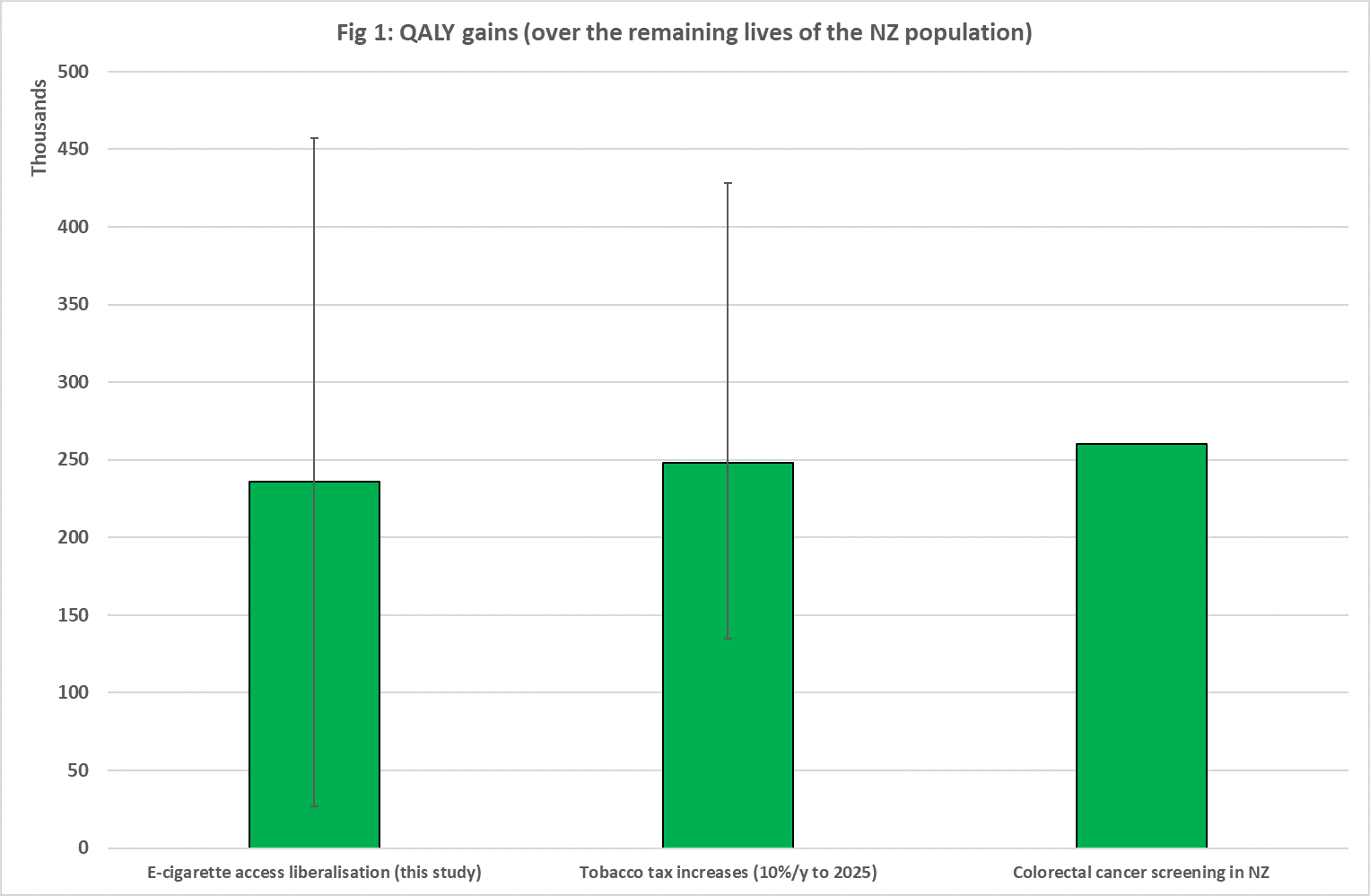
The results were that the NZ population alive in 2011 was estimated to gain 236,000 extra years of healthy life over the remainder of the population’s lifespan – albeit with a wide range whereby 95% of our estimates fell in the range of 27,000 to 457,000 years given all the uncertainties around benefits and harms [1] (all results at 0% discount rate). Over this time period there would also be cost-savings to the NZ health system from a reduction in tobacco-related diseases of NZ$3.4 billion [b] (2011$) (95% range: NZ$370 million to NZ$7.1b). So this intervention has roughly the same health gain as 10% per annum tobacco tax increases per year for 15 years [2], or a national colorectal cancer screening programme [3] (see Fig 1, showing quality-adjusted life-years [QALYs] gained, all using a 0% discount rate).
Note: Error bars are 95% uncertainty intervals
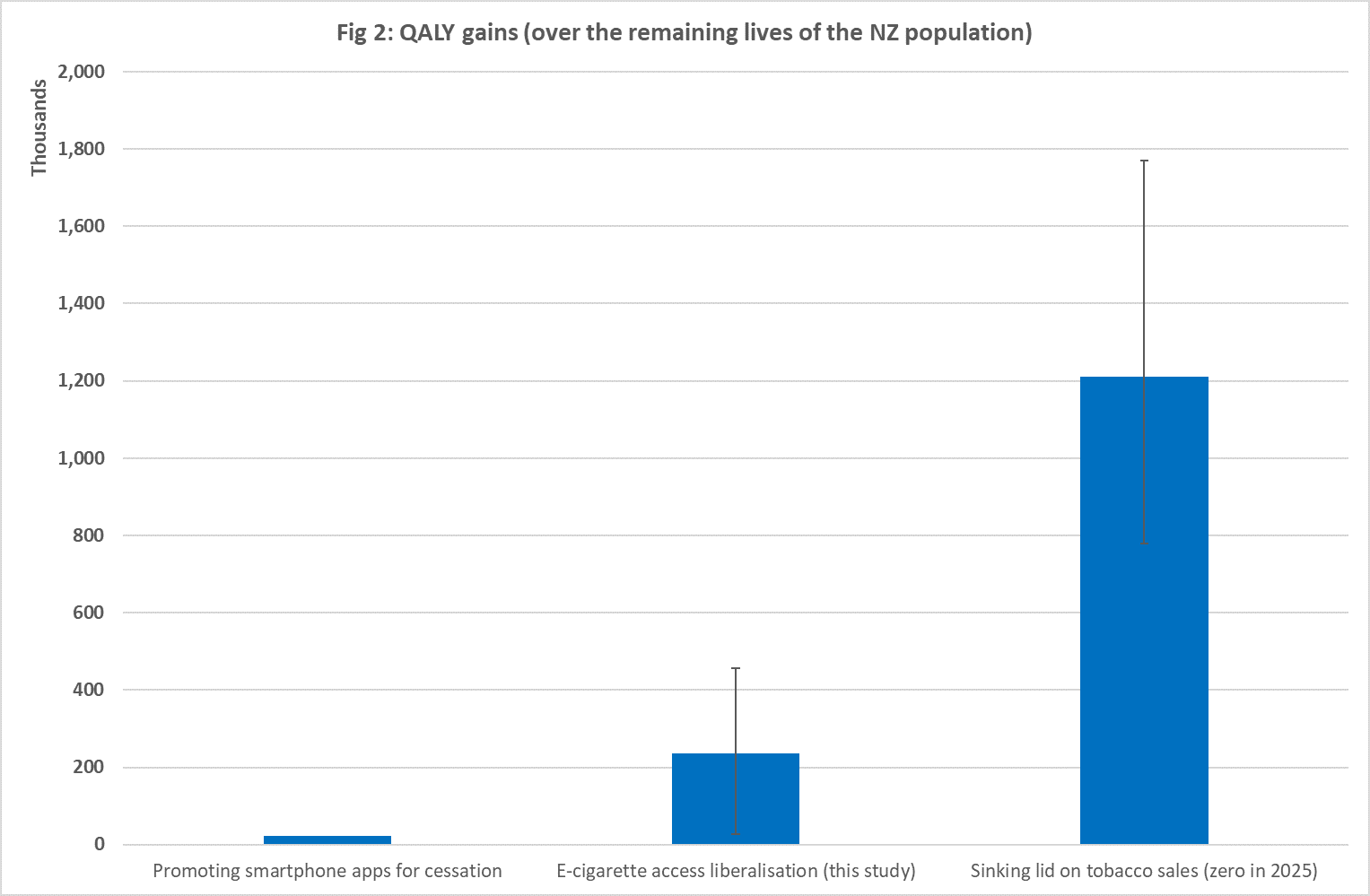
This work can also be compared with the full range of other potential tobacco control interventions we have modelled. It does well when compared to our just published study on the promotion of a smartphone app for smoking cessation (the e-cigarette liberalisation is 10 times better for health gain) [4]. Yet it does fairly poorly compared to a sinking lid on tobacco sales [2] which is 5 times better (see Fig 2, all results at 0% discount rate). For other comparisons see the 29 tobacco control interventions for NZ and Australia that are listed in our online league table at: https://league-table.shinyapps.io/bode3/ (this covers QALY gains, health costs and cost-effectiveness but all results in the league table use a 3% discount rate).
Taking uncertainty into account
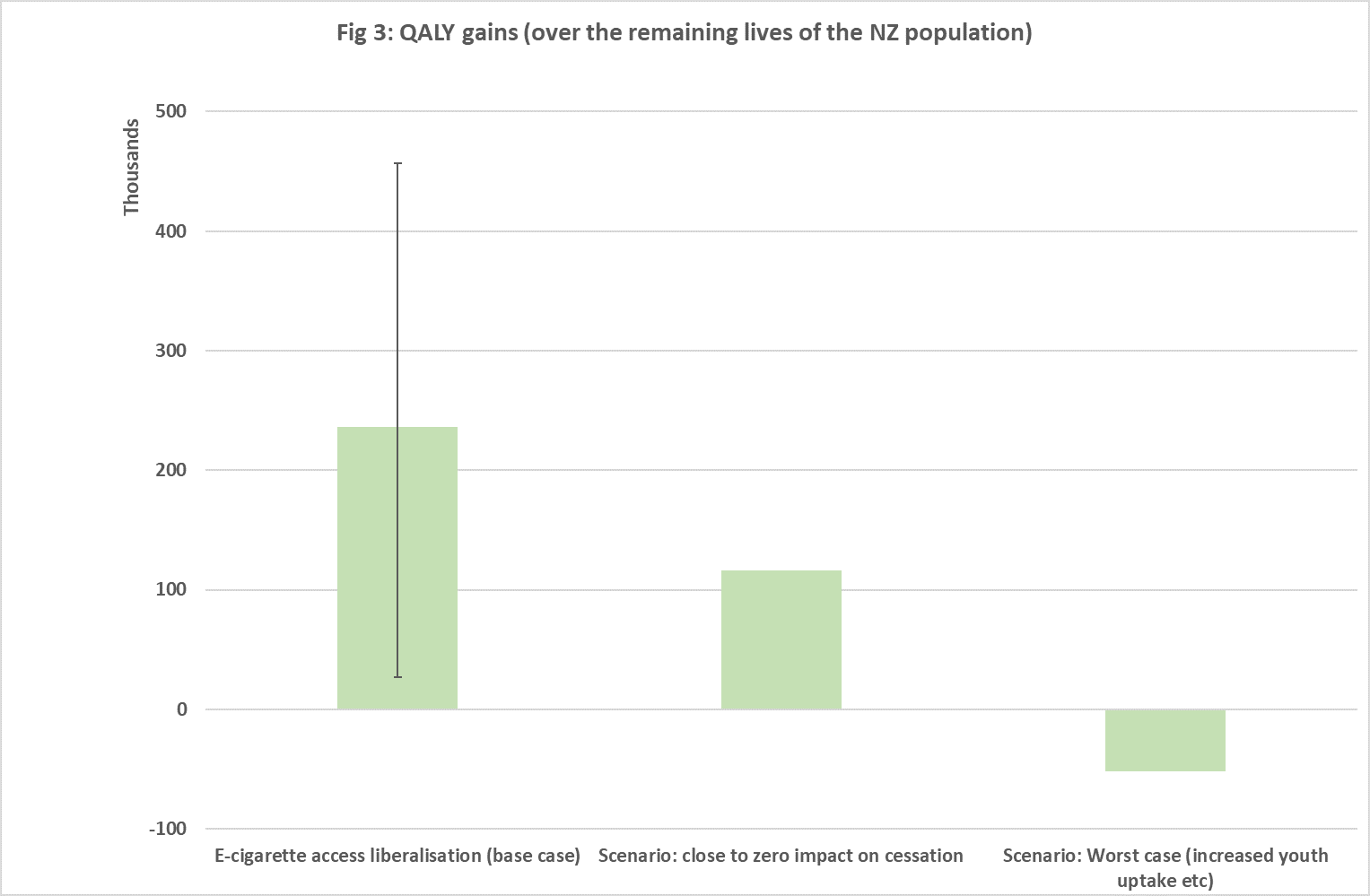
There is genuine scientific uncertainty with our results since there is still a lot that is unknown about vaping and health – and vaping technology is also evolving rapidly. But an advantage of modelling is that we can include uncertainty about many key inputs. That is why when we consider all the major sources of uncertainty in the data that we estimate a 95% uncertainty range for the health gain of between 27,000 and 457,000 healthy years of life. Our study included various scenarios – including a worst case one that assumed “close to zero cessation impact, 38% of smoking health risk of vaping, and an increase in youth smoking uptake rates”. This, albeit very unlikely scenario, resulted in a net loss in health (Fig 3).
But since we submitted our model results for publication, new evidence has emerged which addresses two of the biggest drivers of the uncertainty in the model. This increases our confidence in the base case results. First, a large randomised controlled trial in the UK [5] found that e-cigarettes used during a quit attempt doubled a person’s chance of successful quitting, compared to ‘just’ using standard nicotine replacement therapy (and with both groups getting behavioural support). Second, there are concerns that e-cigarettes may act as a ‘gateway’ for youth to take up tobacco smoking. But examination of the youth tobacco smoking rates since e-cigarette use has increased (eg, in the US [6]), has found no slowing down in the ongoing declines in youth tobacco smoking rates.
Smart regulation should increase health gains and lower vaping-related risks further
NZ currently has the opportunity to build on its history of successful regulation of many aspects of tobacco (marketing, warning labels etc) and relatively tight regulation of prescription medicines, to design appropriate regulations for vaping products. Suggestions we make include: the desirability of avoiding excise taxes on vaping products (so they are cheaper than more harmful tobacco products); combining vaping product sales with smoking cessation advice; ensuring retailers of vaping products – particularly sales staff – are trained in providing advice on dose and other aspects; and on regulations that may reduce youth uptake of vaping [1]. Some of us have published articles on vaping regulation [7] [8] [9] [10] and written various scholarly blogs eg, here, here, and here]. So when the NZ Government commences the Select Committee process for e-cigarette regulations (perhaps later this year) – we hope to present on this work in more detail.
In summary our modelling work suggests that the continuing use of e-cigarettes by New Zealanders (instead of tobacco) will generate large health gains and cost savings to the health system. But there is genuine scientific uncertainty – and more research will be needed to clarify the true size of the health gains. However, we have a high degree of confidence that careful liberalisation of access to e-cigarettes will generate health gain – and likely large health gain. But e-cigarettes are no panacea – much larger gains, perhaps 20 times higher, would be achieved by a ban on commercial combustible tobacco products phased in over a period of time (eg, a sinking lid on supply). Greater availability of lower risk alternative nicotine products, such as e-cigarettes, is also likely to increase the viability of implementing more radical approaches such as phasing out commercial combustible tobacco sales.