Summary
In Aotearoa New Zealand, poor-quality food contributes significantly to diseases like cancer, heart disease, and diabetes, affecting a growing number of people who struggle to afford nutritious diets.
Recent research from Te Rōpū Rangahau ō Te Kāhui Matepukupuku (Cancer Society Research Collaboration) reveals that 84% of New Zealanders support government intervention to reduce the cost of healthy food. Additionally, 73% back free healthy school lunches, and 64% endorse a sugary drinks tax if the revenue supports affordable and available healthy food.
The study underscores the public’s expectation of political action on this front, challenging the misconception that such policies would be unpopular. Such policies should be part of a comprehensive New Zealand Food Strategy, drawing inspiration from successful models overseas.
Poor quality food is a major cause of ill-health and deaths from diseases such as cancer, heart disease, and diabetes in Aotearoa New Zealand. An increasing number of New Zealanders cannot afford to buy a range of fruits, vegetables and unprocessed foods needed for a healthy diet.
Better diets mean not only healthier and longer lives for New Zealanders, but also downstream benefits for healthcare costs, productivity and education and, if implemented well, could reduce health inequities between Māori and non-Māori.
New research shows the people of Aotearoa expect more from politicians on this front. The majority of New Zealanders support more government action on reducing the cost of healthy food, and back policies such as healthy lunches in schools and a tax on sugary drinks.
That is just one of the takeaways from a recent report from Te Rōpū Rangahau ō Te Kāhui Matepukupuku (Cancer Society Research Collaboration).1 Researchers at the University of Otago conducted a representative survey of 1425 adult New Zealanders (details in Appendix), asking them about their knowledge of the impact of alcohol and diet on cancer risk – but also where they stood on several policies put forward as ways to improve the food environment in Aotearoa.
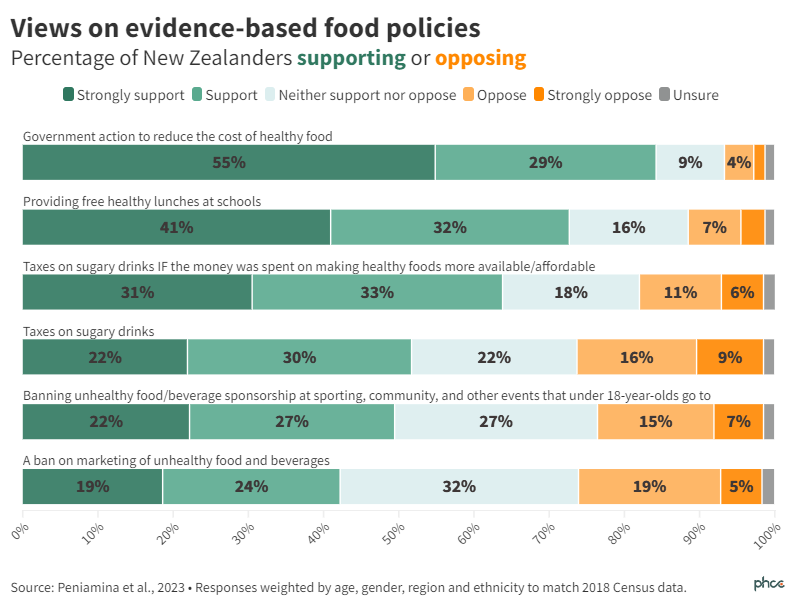
The results show 84% of New Zealanders support government action to reduce the cost of healthy food. There was also strong support for free healthy lunches in schools, with 73% of Kiwis expressing support for this policy.
Just over half (52%) supported a tax on sugary drinks, but this figure jumped to 64% if the revenue from such a tax was used to support making healthy food more available and affordable. Notably, only 17% were opposed to this policy if the revenue was used to improve the availability and affordability of healthy food. Such policies are supported by evidence2 and have worked overseas. Research shows that a 10% tax results in 10% reduction in consumption.2 Sugary drinks taxes are in effect in more than 100 countries and territories impacting 57% of the world’s population, but not in Aotearoa New Zealand. The UK Conservative Government recently introduced such a tax.
Support for banning unhealthy food sponsorship at sports, community, and other events attended by children (49%) and banning marketing of unhealthy food and drinks (43%) was lower but still outweighed opposition substantially.
The importance of clear communication
The survey also highlighted the importance of understanding how food influences health. Overall public awareness of how diet can influence cancer risk was low among those surveyed. For example, half the respondents said they were unsure or didn’t know of any food or drink that could potentially decrease cancer risk. Those who were more aware of the ways in which diet can increase cancer risk (for example knowing that processed meat was a risk factor for cancer) were more likely to support all policies. This suggests that raising public awareness of how our diets can affect cancer risk could build even more public support for policies to improve the food environment. Educational campaigns can also inform healthier choices about food, but this can only happen in a supportive environment which makes the healthy choice the easy choice.
Beyond this, research has shown that clearer communication of the evidence supporting such policies can boost support3,4, as can communicating that there are multiple benefits of policies.5,6
Thus, while it is not the only factor, clear communication of food policy evidence, effectiveness and impact is a crucial step towards better management of the food environment in Aotearoa.
The report’s findings provide a clear mandate to the new Government to act. This includes actions such as aiding the introduction of a third supermarket to keep the price of food down; continuing and strengthening the lunches in schools programme; and introducing a sugary drinks tax. It is important that this kind of research is conducted and clearly communicated to the public and policy makers to show the public support for government action to improve the price and availability of healthy food in Aotearoa.
Getting strategic about food policy
These polices are achievable now and the Government should not delay. Ideally this would form part of a wider food and nutrition strategy. Indeed a collection of National Science Challenges experts have issued a call for a New Zealand Food Strategy.7 Such a strategy would chart a clear way forward for improving food policy in New Zealand and ensure that multiple lines of policy work and implementation are working in concert towards clearly defined goals. We have already seen the United Kingdom, Australia and Canada put in place such overarching plans.
However, the development of a strategy should not preclude immediate action. The incoming government must make policies that improve New Zealand’s food environment and equitable access to healthy food a priority in recognition of the public support for such policies.
What is new in this Briefing?
- New survey research shows a majority of New Zealanders want more government action on reducing the cost of healthy food.
- There is broad public support for, and little opposition to several food policies, including free healthy school lunches and a tax on sugary drinks.
- People with more awareness of dietary risk factors for cancer were more likely to support policies.
Implications for policy
- The Government has a mandate for action with strong public support for healthy food policies.
- Food policies should be implemented as soon as possible and ideally as part of a wider food and nutrition strategy. These include:
- Find ways to reduce the cost of healthy food eg, aiding the introduction of a third supermarket in Aotearoa.
- Continue and strengthen the Ka Ora Ka Ako Lunches in Schools Programme by committing to baseline funding and expanding the programme to 50% of schools.
- Introduce a sugary drinks tax in line with international best evidence.
Author details
Dr Rana Peniamina, Research Fellow, Te Rōpū Rangahau ō Te Kāhui Matepukupuku: Cancer Society Research Collaboration, Department of Preventive and Social Medicine, University of Otago, Dunedin
Dr Bronwen McNoe, Co-Director of Te Rōpū Rangahau ō Te Kāhui Matepukupuku: Cancer Society Research Collaboration, Department of Preventive and Social Medicine, University of Otago, Dunedin
Dr John Kerr, Science Lead, Public Health Communication Centre, Department of Public Health, University of Otago, Wellington
Dr Cristina Cleghorn, Senior Research Fellow, Department of Public Health, University of Otago, Wellington
Prof Louise Signal, Co-Director of Te Rōpū Rangahau ō Te Kāhui Matepukupuku: Cancer Society Research Collaboration, Department of Public Health, University of Otago, Wellington
Acknowledgements
This research was supported by a grant from the Cancer Society of New Zealand.
Appendix: Survey methods
Taken from the original report: Public awareness of cancer risk factors & support for prevention policies in Aotearoa New Zealand: A focus on alcohol and diet.
The current research sought to determine New Zealanders’ awareness of modifiable risk factors for cancer (with a particular focus on alcohol and dietary factors) and support for evidence-based alcohol and food policies to reduce people’s exposure to alcohol and dietary risk factors in their environment. A survey instrument was developed based on previous research. It was included in a self-administered online omnibus survey run by Talbot Mills Research. Data collection was completed in March-April 2023. A sample of 1425 New Zealanders aged 18 years and older were recruited by panel provider DynataTM, which included a representative sample of 1000 New Zealanders and boosted sampling for Māori and Pasifika people to provide equal explanatory power for these population groups.
Survey responses were weighted (through post-stratification weights) to ensure that they represented, as closely as possible, the Aotearoa adult population from the 2018 Census. Recall questions were manually coded into categories. Data analysis was conducted using Stata/SE version 18.0. Logistic regression was used to determine if significant differences were evident in responses to the recognition risk factor awareness question and the policy support questions (outcomes), based on specified independent variables.
This article is part of the series Briefings to the Incoming Government, highlighting challenges and opportunities in the public health policy space.